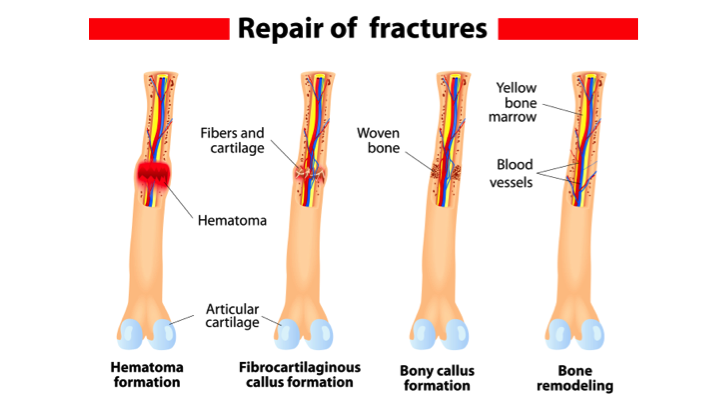
This new bony callus is also called the hard callus. The cartilage in the calluses is replaced by trabecular bone via endochondral ossification (destruction of cartilage and replacement by bone) ( Figure 6.5.2 c). Over the next several weeks, osteoclasts resorb the dead bone while osteogenic cells become active, divide, and differentiate into more osteoblasts. Together, these temporary soft calluses stabilize the fracture. Additionally, the periosteal chondrocytes form and working with osteoblasts, create an external callus of cartilage and bone, respectively, around the outside of the break ( Figure 6.5.2 b). Within about 48 hours after the fracture, stem cells from the endosteum of the bone differentiate into chondrocytes which then secrete a fibrocartilaginous matrix between the two ends of the broken bone gradually over several days to weeks, this matrix unites the opposite ends of the fracture into an internal callus (plural = calli or calluses). (d) Remodeling occurs to replace immature bone with mature bone. (c) Cartilage of the calluses is gradually eroded and replaced by trabecular bone, forming the hard callus. (b) Internal and external calluses form made of cartilage and bone. Figure 6.5.2 – Stages in Fracture Repair: The healing of a bone fracture follows a series of progressive steps: (a) Broken blood vessels leak blood that clots into a fracture hematoma. Though broken vessels promote an increase in nutrient delivery to the site of vessel injury (see inflammation process in blood vessel chapter), the disruption of blood flow to the bone results in the death of bone cells around the fracture. In this process, blood released from broken or torn vessels in the periosteum, osteons, and/or medullary cavity clots into a fracture hematoma ( Figure 6.5.2 a). With indirect bone healing the process is more complicated and similar to endochondral bone formation in which broken bones form cartilaginous patches before regrowing new bone. Direct bone healing is essentially bone remodeling in which osteoblasts and osteoclasts unite broken structures. One fragment is driven into the other, usually as a result of compressionĪ partial fracture in which only one side of the bone is broken, often occurs in the youngĪ fracture in which at least one end of the broken bone tears through the skin carries a high risk of infectionĪ fracture in which the skin remains intactĭepending on the type, severity of the fracture and distance between bone fragments, bones may heal directly by building new bone onto the fracture site (direct bone healing or contact healing) or may heal in a process like endochondral bone formation (indirect bone healing). Several breaks result in many small pieces between two large segments Occurs at an angle that is not 90 degreesīone segments are pulled apart as a result of a twisting motion Occurs straight across the long axis of the bone Figure 6.5.1 – Types of Fractures: Compare healthy bone with different types of fractures: (a) open fracture, (b) closed fracture, (c) oblique fracture, (d) comminuted fracture, (e) spiral fracture, (f) impacted fracture, (g) greenstick fracture, and (h) transverse fracture. Some fractures may be described using more than one term because it may have the features of more than one type (e.g., an open transverse fracture). Table 6.4 outlines common types of fractures. 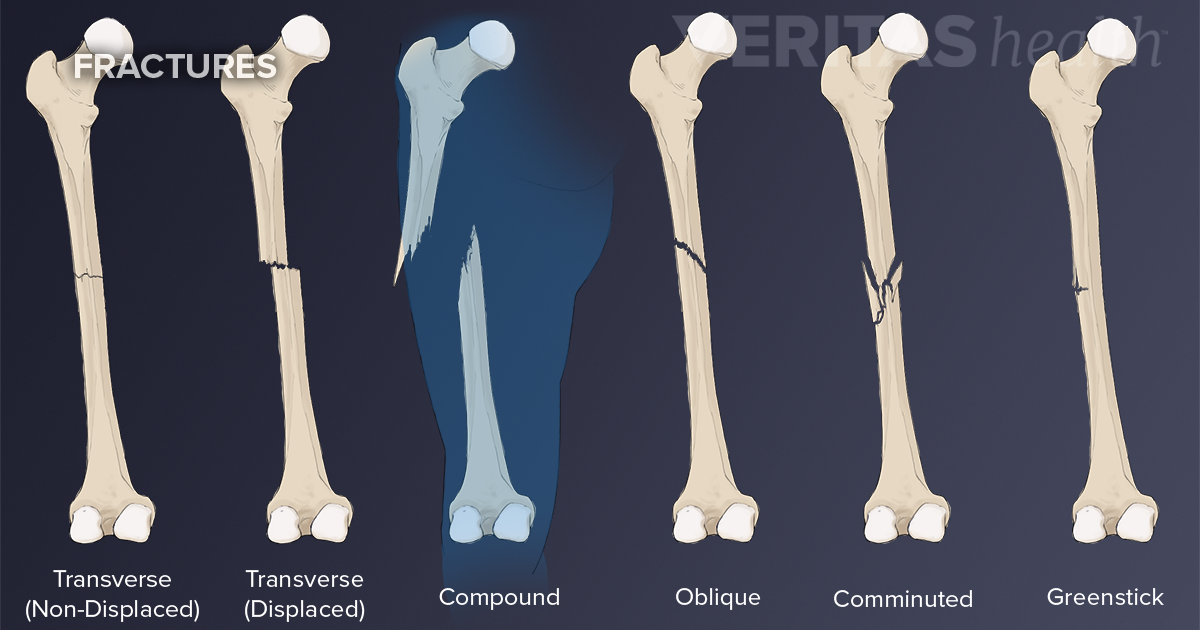
Types of Fracturesįractures are classified by their complexity, location, and other features ( Figure 6.5.1). These can become lodged in the capillary beds of the lungs, leading to respiratory distress and if not treated quickly, death (this is called a pulmonary embolism). 
For example, a fractured diaphysis of the femur has the potential to release fat globules into the bloodstream. While some fractures can be minor, others are quite severe and result in grave complications. Open reduction requires surgery to expose the fracture and reset the bone. When a broken bone is manipulated and set into its natural position without surgery, the procedure is called a closed reduction. If the bone is not reset correctly, the healing process will rebuild new bone but keep the bone in its deformed position. It will heal whether or not a physician resets (places) it in its anatomical position.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
